ARTICLE REVIEW
ROSA, Deborah Fonseca [1], MARQUES, Sandy Lorrayne Rodrigues Cardoso [2], CAIXETA, Victor Fernandes Gaspar [3], KALLÁS, Adriane da Rocha [4], FRADE, Rodrigo Itaboray [5], OLIVEIRA, Sabrynna Brito [6]
ROSA, Deborah Fonseca. et al. Reflections on the difficulties in treating gestational syphilis: from the patient to the health system. Revista Científica Multidisciplinar Núcleo do Conhecimento. Year 08, Ed. 07, Vol. 04, pp. 05-16. July 2023. ISSN: 2448-0959, Access Link: https://www.nucleodoconhecimento.com.br/health/difficulties-in-treating, DOI: 10.32749/nucleodoconhecimento.com.br/health/difficulties-in-treating
ABSTRACT
Syphilis, an infection caused by the bacterium Treponema pallidum, is a worldwide systemic disease with a chronic course that affects only humans as its host. Transmission can occur through sexual or vertical means. Newborns of mothers with untreated syphilis or those who did not undergo proper treatment may present with either an asymptomatic or severe systemic symptoms. The aim of this study was to conduct a literature review on patient behavioral factors and public health actions that can impact the treatment of gestational syphilis. Articles published in Portuguese, available in full text in the databases Medline, Scielo, Biblioteca Virtual da Saúde (BVS), Lilacs, and PubMed, were considered. Official publications from the Ministry of Health within the same time frame were also taken into account. The results indicate that the main difficulties related to the treatment of gestational syphilis include: deficiencies and/or lack of prenatal care; a shortage of information aimed at pregnant women about the disease; limited access to the primary medication or a failure to seek it; limited adherence of partners to treatment and the use of condoms in sexual relationships. It is necessary to adjust prevention campaigns and monitoring/treatment follow-up for syphilis cases in pregnant women to reduce the negative impact on public health of a treatable and curable disease.
Keywords: Syphilis, Congenital Syphilis, Infectious Pregnancy Complications.
1. INTRODUCTION
According to the Ministry of Health – MS (2020), syphilis is a global infectious and systemic disease, considered one of the main Sexually Transmitted Infections (STIs). The etiological agent is the bacterium Treponema pallidum, which has humans as the only host, transmitter, and reservoir.
Syphilis can be transmitted in various ways, with the main modes being horizontal transmission, where there is unprotected sexual contact with an infected person, direct contact with the genital mucosa, blood, or saliva of infected individuals – clinically classified as acquired syphilis; and vertical transmission, where an infected pregnant woman transmits the infection to the fetus during pregnancy – clinically classified as congenital syphilis (BRASIL, 2020; KALININ; NETO; PASSARELLI, 2015).
The manifestations of syphilis are independent of the affected population and are classified according to the disease’s progression into primary, secondary, tertiary, and latent syphilis, with a higher risk of transmission in the primary and secondary presentations. After the incubation period, which varies between ten days and three months, the first symptoms appear: a painless lesion at the site of bacterial entry, with a hardened base and serous discharge, also called a hard chancre (MARQUES et al., 2018).
According to MS (2010), in most cases, the primary lesion spontaneously heals within two weeks. However, when syphilis is not treated during the primary stage, it progresses to secondary syphilis. At this stage, the bacterium has already invaded all organs and fluids of the body, and the individual presents with a skin rash, macules, papules, or large white-grayish erythematous plaques called condyloma lata, which can appear on the body’s mucous membranes.
Failure to treat secondary syphilis can progress to a latent infection, considered ‘early’ within the first year and ‘late’ after that period. Latent syphilis does not exhibit any clinical manifestations. After entering latency, syphilis can take decades to manifest, appearing in its tertiary form. The main manifestations include inflammation and tissue and bone destruction, as well as more severe cardiovascular and neurosyphilis manifestations (BRASIL, 2010).
According to data from the Notifiable Diseases Information System (SINAN), between 2005 and 2020, approximately 380,000 cases of syphilis in pregnant women were recorded in Brazil, with the Southeast and Northeast regions having the highest number of cases (45.3% and 20.9%, respectively) (BRASIL, 2020).
Early diagnosis and treatment of gestational syphilis prevent the infection from affecting various organs of the body, such as the nervous system, heart, bones, skin, and eyes (MARQUES et al., 2018). Additionally, there is a possibility of transmission to the fetus, increasing the risk of prenatal complications by 4.5 times when compared to uninfected pregnant women (GOMEZ et al., 2013). If not properly treated, congenital syphilis can lead to spontaneous abortion, premature birth, fetal and neonatal death (MAGALHÃES et al., 2011). Newborns of mothers with untreated or inadequately treated syphilis can either be asymptomatic or develop late-onset symptoms, causing serious damage to their physical health, as well as psychological and social repercussions (MACÊDO, 2017).
Two crucial aspects regarding disease control are prevention and diagnosis. The first is to prevent an increase in disease incidence, and the second is to initiate treatment in the early stages, reducing associated complications (MASCARENHAS, 2016).
Despite the cure for gestational syphilis being available, its diagnosis being simple, and treatment being effective and affordable, the number of cases of gestational syphilis and associated complications still exceeds the recommendations of health organizations. Based on this, the present study aimed to understand the primary patient behavioral factors and public health actions that negatively affect the treatment of gestational syphilis.
2. MATERIALS AND METHODS
The present descriptive study was conducted through an exploratory research of publications released between 2006 and 2021. Initially, the time series was restricted to the last 5 years; however, due to the lack of published materials, the publication interval was extended.
The stages of the screening process and selection of bibliographic material are outlined in Figure 1.
Figure 1. Methodology used by the authors: stages of the screening process and selection of bibliographic material
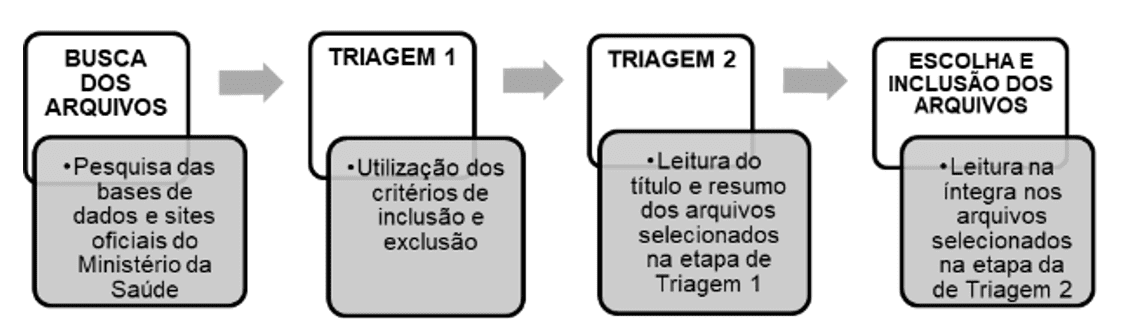
The first stage involved searching for publications using the following databases as a basis: Medical Literature Analysis and Retrieval System Online (Medline), Scientific Electronic Library Online (Scielo), Biblioteca Virtual em Saúde (BVS), Lilacs, PubMed, and the Ministry of Health (MS). For this research, the terms ‘Sífilis,’ ‘Sífilis congênita,’ ‘Complicações Infecciosas na Gravidez,’ and words related to the topic, such as ‘tratamento,’ ‘gestação,’ ‘pré-natal,’ ‘abandono do tratamento de sífilis em grávidas,’ ‘sífilis em grávidas,’ ‘complicações da sífilis gestacional,‘ among others, were used.
For the initial screening of the found texts, inclusion and exclusion criteria were applied. Articles, undergraduate theses, and dissertations published in Portuguese, as well as official publications on this topic by the Ministry of Health, were considered. Materials published before 2006, those not available in full text, and those published in a language other than Portuguese were not included in this research.
In screening stage 2, the title and abstract of the works were read to confirm the selection criteria and to ensure that the material was relevant to the research topic. The final collection was assembled after reading the pre-selected works in their entirety.
The bibliographic collection for this review consisted of 35 titles, including 22 articles, 2 dissertations, 2 undergraduate theses, 3 books, and 6 epidemiological bulletins from the Ministry of Health.
3. RESULTS
During the conducted research, a sequence of important findings was established regarding the factors that negatively impact the treatment of gestational syphilis. Conditions associated with the treatment failure of gestational syphilis were identified, including lack of pregnant women’s knowledge about the disease, failure to undergo prenatal exams, inadequate and/or insufficient prenatal care and diagnosis, missed medical appointments, lack of access to or discontinuation of treatment, absence of preventive education, untreated infected partners, limited access to healthcare, low socioeconomic status, among others (DOMINGUES et al., 2013; GALATOIRE et al., 2012). These factors were categorized and detailed into three topics, namely: factors associated with the pregnant woman and her partner, factors related to healthcare services, and health education.
3.1 OF THE PREGNANT WOMAN AND HER PARTNER
Most people with syphilis are unaware of their infection, thus becoming potential transmitters to their sexual contacts. This happens due to the absence or scarcity of symptoms, depending on the stage of the infection (BRASIL, 2016).
According to Gomes et al. (2021), there are many factors that can contribute to pregnant women being vulnerable to Treponema pallidum infection, such as a lack of information about the complications of syphilis during pregnancy, non-use or improper use of condoms during sexual relations during pregnancy, a lack of confidence in discussing this issue with their partner, and individual factors like the pregnant woman’s low socioeconomic status and level of education.
The authors also note that pregnant women’s knowledge about syphilis is limited to understanding that it’s a type of Sexually Transmitted Infection (STI) that can be prevented through barrier methods and has a rapid test for detection. However, pregnant women do not seem to have knowledge about vertical transmission and risks to the baby, indicating their lack of awareness of the complications (GOMES et al., 2021).
Equally important, the partner’s neglect in the treatment of gestational syphilis also influences the success of treating the condition (COSTA et al., 2017). The use of a condom is necessary during sexual intercourse to prevent the pregnant woman from becoming infected for the first time during pregnancy or even re-infection (SILVA & BONAFÉ, 2013). Therefore, it is essential for the partner to also participate in screening and monitoring certain health conditions during pregnancy, including syphilis.
3.2 OF HEALTHCARE SERVICES
Early in pregnancy, closer monitoring of the expectant mother is necessary to ensure that she is healthy to proceed with the pregnancy. This includes assessing various habits and the presence of any pathologies or physiological alterations that may compromise the health of the pregnant woman and the developing child (COSTA et al., 2017).
Public healthcare services should provide support to pregnant women from diagnosis to the treatment of gestational syphilis. Hence, the difficulties in achieving successful and proper treatment are also linked to the lack of access to public healthcare services, the failure to perform serological tests on pregnant women, and the absence of treatment and/or partner monitoring (FRANÇA et al., 2015).
It is essential to detect syphilis during prenatal care so that both the mother and the baby can receive timely and adequate treatment. When left untreated, syphilis can progress to more severe forms, often affecting the nervous and cardiovascular systems (BRASIL, 2016).
According to Macêdo et al. (2020), vertical transmission of syphilis still occurs due to late initiation of prenatal care, delays in requesting tests and obtaining their results, as well as the waiting time for follow-up appointments. Furthermore, the authors note that prenatal care has shortcomings resulting in low appropriateness and a predominance of partially implemented actions.
In Brazil, despite the high coverage of prenatal care, there is a lack of monitoring and appropriateness of assistance. Pregnant women with no prenatal visits or an insufficient number of visits are observed, particularly among young and low-educated women (PEREIRA et al., 2020).
The absence or inadequacy of prenatal care negatively impacts the treatment of gestational syphilis since it can lead to delays in disease treatment and harm the health of both the mother and the fetus. Furthermore, the absence of prenatal care prevents the doctor from continuing the treatment of previously diagnosed syphilis (MASCARENHAS et al., 2016).
The lack of access to medication or its incorrect use can also be cited as an important factor that can lead to the exacerbation or possible transmission of syphilis from mother to child. This is because, even though penicillin is a medication that is distributed free of charge in health centers, depending on the region where the pregnant woman resides and her level of awareness about the disease and its consequences, lack of access to medication or negligence in its use can allow the condition to progress, leading to irreversible consequences for both the mother and the child (MASCARENHAS et al., 2016).
Additionally, in the case of gestational syphilis, early treatment can reduce the chances of affecting the baby and causing harm to their health. The most significant complication of gestational syphilis is the lack of proper treatment, or in some cases, the absence of treatment (GONÇALVES et al., 2020).
3.3 OF HEALTH EDUCATION
The lack of information and the difficulty of accessing specialized services are present as contributing factors to inadequate treatment or even a lack of treatment (MASCARENHAS et al., 2016; BONI, PAGLIARI, 2016; FELIZ et al., 2016).
The absence of knowledge about syphilis and/or the lack of access to information can complicate and/or worsen the infection, as the later the start of treatment, the longer and more prolonged the healing process will be (GONÇALVES et al., 2020).
It is necessary to emphasize the approach to STIs for women so that pregnant women can acquire knowledge that encompasses the spread of health problems, the importance of therapeutic treatment, and prevention of vertical transmission of diseases. Regarding gestational syphilis, public policies are needed to promote awareness and training of prenatal care professionals, especially for managing the disease during pregnancy (GOMES et al., 2021).
Guidance for women and their partners on safe sexual practices is essential, promoting a primary healthcare intervention for these pregnant women and eradicating syphilis transmission factors (GOMES et al., 2021).
4. FINAL CONSIDERATIONS
Among the main behavioral factors that hinder the treatment of gestational syphilis, the following stand out: the absence or failures during prenatal care, which negatively influence the treatment of gestational syphilis, leading to late diagnosis or treatment abandonment, even with instructions for exams and drugs to control the disease’s presence.
Neglect or the pregnant woman’s failure to address the issue with her partner in the treatment of syphilis are factors that influence the success of treating the condition, as well as the importance of prevention during sexual activity. If there is unprotected intercourse, it is essential to undergo tests to check for infection with the Treponema pallidum bacterium.
Regarding education and public health, public policies are needed to promote awareness and training of prenatal care professionals, especially for managing the disease during pregnancy. It is necessary to emphasize women’s approach to STIs so that pregnant women can acquire knowledge that encompasses the spread of health problems, the importance of therapeutic treatment, and prevention of vertical transmission of diseases.
Furthermore, awareness efforts should be extended to the partners of those affected by the disease to ensure that treatment is conducted jointly and to prevent re-infection of the pregnant woman in an effort to preserve the health of both parents and the child.
In addition, it is important for healthcare professionals to take more actions to raise awareness about the disease and its prevention and treatment methods, as well as to encourage prenatal care, as many mothers tend to seek care too late. In this case, it is crucial to start as early as possible to increase the chances of successful treatment and promote the health and development of the fetus.
Considering these challenges, there is a clear need for more comprehensive actions targeting the population, demonstrating the risks associated with gestational syphilis for both the pregnant woman and the fetus. Finally, it is believed that technology and the speed of information dissemination could be used to educate the population about the prevention and treatment of gestational syphilis.
The main limitation of this research was the availability of updated scientific literature on the topic, which hindered more current or interconnected reflections on the findings. Therefore, it is suggested that this topic be addressed with up-to-date and targeted approaches for pregnant women receiving care through the public health system (SUS) throughout the country.
ACKNOWLEDGMENTS
The authors would like to thank the professors at the Izabela Hendrix University Center, Alfonso Gala Garcia and Rafaela de Oliveira Silva, for their contributions during the writing of this article, which was the result of the authors’ thesis work.
REFERENCES
BRASIL. Ministério da Saúde. Manual Técnico para Diagnóstico da Sífilis. Secretaria de Vigilância em Saúde Departamento de Vigilância, Prevenção e Controle das Doenças Sexualmente Transmissíveis, Aids e Hepatites Virais. Brasília, 2016. Disponível em: http://vigilancia.saude.mg.gov.br/index.php/download/manual-tecnico-para-diagnostico-da-sifilis-2016/?wpdmdl=7704. Acesso em: 10 Jun. 2021
BRASIL. Ministério da Saúde. Secretaria de Vigilância em Saúde. Boletim Epidemiológico: Sífilis. Brasil, 2020. Disponível em: http://www.aids.gov.br/pt-br/tags/publicacoes/boletim-de-sifilis. Acesso em: 07 Jun. 2021
BRASIL. Ministério da Saúde. Sífilis: Estratégias para Diagnóstico no Brasil. Brasília: Ministério da Saúde, Coordenação de Doenças Sexualmente Transmissíveis e Aids, p. 100. 2010 (Série TELELAB). Disponível em : https://bvsms.saude.gov.br/bvs/publicacoes/sifilis_estrategia_diagnostico_brasil. Aceso em: 29 Jul. 2022
BONI, Sara Macente; PAGLIARI, Priscila Bertoncello. Incidência de sífilis congênita e sua prevalência em gestantes em um município do noroeste do Paraná. Rev. Saúde e Pesquisa, Maringá, v. 9, n. 3, p. 517-524, 2016. Disponível em: http://periodicos.unicesumar.edu.br/index.php/saudpesq/article/view/5530/2919. Acesso em: 13 Abr. 2021.
COSTA, Carolina et al. Sífilis congênita: repercussões e desafios. Arquivos Catarinenses de Medicina, v. 46, n. 3, p. 194-202, 2017. Disponível em: https://www.unirv.edu.br/conteudos/fckfiles/files/09%20S%c3%8dFILIS%20Artigo%20publicado%20agosto%202017. Acesso em: 19 Abr. 2021
DOMINGUES, Rosa Maria Soares Madeira et al. Sífilis congênita: evento sentinela da qualidade da assistência pré-natal. Rev. Saúde Pública, São Paulo, v. 47, n. 1, p. 147-157, 2013. Disponível em: https://www.scielo.br/j/rsp/a/bsJrGNxmFyqqdNKtGSDjxhz/?lang=pt&format=pdf. Acessos em: 16 Maio. 2020.
FELIZ, Marjorie Cristiane et al. Aderência ao seguimento no cuidado ao recém-nascido exposto à sífilis e características associadas à interrupção do acompanhamento. Rev. Brasileira de Epidemiologia, São Paulo, v. 19, n. 4, 2016. Disponível em: https://www.scielo.br/j/rbepid/a/5q9MDTSqYndgvgMBLBxxsVK/?lang=pt&format=pdf. Acesso em: 13 Abr. 2021.
FRANÇA, Inacia Sátiro Xavier de et al. Fatores associados à notificação da sífilis congênita: um indicador de qualidade da assistência pré-natal. Rev. Rene, v. 16, n. 3, p. 374-381, 2015. Disponível em: http://www.periodicos.ufc.br/rene/article/view/2805/2174. Acesso em: 13 Abr. 2021.
GALATOIRE, Pamela Sue Aranibar; ROSSO, José Antônio; SAKAE, Thiago Mamôru. Incidência de sífilis congênita nos estados do Brasil no período de 2007 a 2009. Arquivo Catarinense de Medicina, v. 41, n. 2, p. 26-32, 2012.
Disponível em: http://www.acm.org.br/acm/revista/pdf/artigos/924.pdf. Acesso em: 22 Abr. 2021.
GOMEZ, Gabriela B et al. Untreated maternal syphilis and adverse outcomes of pregnancy: a systematic review and meta-analysis. Bull World Health Organ, Amsterdam, v. 91, n. 3, 2013. Disponível em: https://pubmed.ncbi.nlm.nih.gov/23476094/. Acesso em: 26 Jun. 2020
GOMES, Natália et al. “Só sei que é uma doença”: conhecimento de gestantes sobre sífilis. Revista Brasileira em Promoção da Saúde, [S. l.], v. 34, 2021. Disponível em: https://periodicos.unifor.br/RBPS/article/view/10964. Acesso em: 18 Abr. 2021.
GONÇALVES, Maria Marly et al. Os Desafios no Tratamento da Sífilis Gestacional. Rev. Multidisciplinar e de Psicologia, v. 14, ed. 49, p.106-113, 2020. Disponível em: https://idonline.emnuvens.com.br/id/article/view/2323. Acesso em: 13 Abril. 2021
KALININ, Yuri; NETO, André Passarelli; PASSARELLI, Dulce Helena Cabelho. Sífilis: aspectos clínicos, transmissão, manifestações orais, diagnóstico e tratamento. Rev. Odonto. São Paulo, v. 23, n. 45-46, 2015. Disponível em: https://pesquisa.bvsalud.org/portal/resource/pt/biblio-909279. Acesso em: 26 Junho. 2020
MACÊDO, Vilma Costa de et al. Fatores de risco para sífilis em mulheres: estudo caso-controle. Rev. Saúde Pública. São Paulo, v. 51, 78, 2017. Disponível em: https://www.scielo.br/j/rsp/a/NQhm4fVf7cqDnvDMGQpmGsD/?lang=en&format=pdf. Acesso em: 16 de Maio de 2020.
MACÊDO, Vilma Costa de et al. Sífilis na gestação: barreiras na assistência pré-natal para o controle da transmissão vertical. Cadernos saúde coletiva. v. 28, n. 4, 2020. Disponível em: https://www.scielo.br/j/cadsc/a/VRdb5W4cRvgYCq7gYHcqB4x/?lang=pt&format=pdf Acesso em: 10 Maio. 2021.
MAGALHÃES, Daniela Mendes dos Santos, et al. A sífilis na gestação e sua influência na morbimortalidade materno-infantil. Comunicação em Ciências da Saúde, v. 22, sup. 1, p. 43-54, 2011. Disponível em: http://hdl.handle.net/11449/136931. Acesso em: 16 Maio. 2020
MARQUES, João Vitor Souza, et al. Perfil epidemiológico da sífilis gestacional: clínica e evolução de 2012 a 2017. SANARE – Revista de Políticas Públicas. Sobral, v.17, n. 2, p. 13-20, 2018. Disponível em : https://sanare.emnuvens.com.br/sanare/article/view/1257/665 Acesso em: 29 Jul. 2022
MASCARENHAS, Luciane Eline Ferreira, et al. Desafios no tratamento da sífilis gestacional. Repositório Institucional: Escola Bahiana de Medicina e Saúde Pública, [S. l.], 2016. Disponível em: https://repositorio.bahiana.edu.br:8443/jspui/handle/bahiana/735. Acesso em: 16 Maio. 2020.
PEREIRA, Allana et al. Impacto do grau de escolaridade e idade no diagnóstico tardio de sífilis em gestantes. Revista Femina. São Paulo, v. 48, n. 9, p. 563-567. Disponível em: http://fi-admin.bvsalud.org/document/view/gsusn. Acesso em: 20 de Abril de 2021.
SILVA, Ana Carolina Zschornak da; BONAFÉ, Simone Martins. Sífilis: uma abordagem geral. In: ENCONTRO INTERNACIONAL DE PRODUÇÃO CIENTIFICA CESUMAR, 2013, Maringá. Anais. Maringá: VIII EPCC, 2013. Disponível em: http://www.cesumar.br/prppge/pesquisa/epcc2013/oit_mostra/ana_carolina_zschornak_da_silva.pdf. Acesso em: 07 Jun. 2021.
[1] Bachelor of Biomedical Science. ORCID: https://orcid.org/0000-0001-7034-7008.
[2] Bachelor of Biomedical Science. ORCID: https://orcid.org/0000-0001-7052-4131.
[3] Bachelor of Biomedical Science. ORCID: https://orcid.org/0000-0003-4381-6571.
[4] Bachelor of Biomedical Science. ORCID: https://orcid.org/0000-0002-8836-9624.
[5] Pedagogue and Physicist, Master in Technological Education at the Federal Center for Technological Education of Minas Gerais. ORCID: https://orcid.org/0000-0001-7773-8175.
[6] Supervisor. Biomedical Scientist, Master and Ph.D. in Microbiology, Postdoctoral Fellow in the Department of Preventive Veterinary Medicine – UFMG. ORCID: https://orcid.org/0000-0001-9303-4338.
Submitted: April 26, 2023.
Approved: June 22, 2023.
















