ORIGINAL ARTICLE
CARNEIRO, Larissa Queiroz Costa [1], BARBOSA, Isabela Menezes [2], CARDOSO, Igor de Souza [3], DIAS, Cláudio Alberto Gellis de Mattos [4], OLIVEIRA, Euzébio de [5], DENDASCK, Carla Viana [6], FECURY, Amanda Alves [7]
CARNEIRO, Larissa Queiroz Costa. Et al. Epidemiological profile of patients served due to official accidents in the north of Brazil, Amazon Region, in the period from 2009 to 2019. Revista Científica Multidisciplinar Núcleo do Conhecimento. Year 05, Ed. 09, Vol. 03, pp. 47-59. September 2020. ISSN:2448-0959, Access link in: https://www.nucleodoconhecimento.com.br/health/profile-of-patients, DOI: 10.32749/nucleodoconhecimento.com.br/health/profile-of-patients
ABSTRACT
Ophidian accidents are a significant public health problem worldwide, due to both their frequency and morbidity and mortality. In Brazil, during the years 2009 to 2019 there were 313,139 registered cases, of which 151,565 occurred in the North Region, making explicit the importance of studying this disease in that Region. The objective of the present study is to determine the epidemiological profile of the affected patients (age and sex), the accident itself (UF, month, year, time to attend) and the snake gender of the accidents that occurred in the Northern region of Brazil. Secondary data were obtained through access to the Information Department of the Brazilian Unified Health System (DATASUS), at the electronic address www.datasus.gov.br, in the SIH / SUS Hospital Information System. It was found that the accidents occurred mainly in rural areas, with men, in socioeconomically active age, caused by snakes of the Bothrops genus. Several cases could be classified as accidents at work, these could be avoided or minimized with appropriate personal protective equipment and guidelines.
Keywords: Snakebite, Snake, Amazon, Brazil.
INTRODUCTION
Accidents caused by venomous snakes represent a significant public health problem, especially in tropical countries due to the frequency with which they occur and the morbidity and mortality they cause. So much so that accidents with venomous animals are classified by the World Health Organization as a neglected tropical disease, which implies that they are more common in places of difficult access and in populations with low socioeconomic status (PINHO et al., 2001; WHO, 2019).
Venomous animals are defined as having venomous glands associated with active venom injection mechanisms, such as hollow dentition, stingers and goads. Being represented by several genera and species of snakes, as well as scorpions, kilopods and arachnids. They differ from passive poisonous animals such as taturanas, frogs and lizards, which have mechanisms of contact poisoning, ingestion and compression (GUTIÉRREZ et.al., 2017).
Thus, snakebite accidents are also classified as a medical emergency, and as such, they can quickly lead the victim to death. The effects of poisoning can be local or systemic, and this depends on the species of snake and the toxins present in the poison (WHO, 2019).
Worldwide, about 7,400 people are bitten by snakes daily, however, the most relevant fact is that, of these cases, 220 to 380 people evolve to death. Totaling approximately 140 thousand deaths per year in the world (PINHO et al., 2001; WHO, 2019).
In Brazil, since 1986, the notification of such accidents is compulsory, which are found in the Disease Notification Information System (SINAN), where about 30 thousand complications with snake bites were reported every year in the last decade, with notorious contribution of the North region of the country in these numbers (WEISS; PAIVA, 2017).
AIM
To trace the epidemiological profile of patients treated due to snakebites in northern Brazil, in the Amazon region, in the period from 2009 to 2019, identifying the variables that influenced the occurrence of these accidents.
METHOD
An analytical and retrospective study was carried out, using the spreadsheets generated through the electronic page of the Department of Informatics of the Unified Health System (DATASUS) at www.datasus.saude.gov.br as the data collection instrument, obeying the following steps respectively: “Access to information”; “Health information (TABNET)”; “Epidemiological and Morbidity”; “Diseases and Notifiable Diseases” – from 2007 onwards; “Accidents due to Venomous Animals” e; finally, the option “Brazil by region, state and municipalities”.
The resulting spreadsheets aggregated the following variables provided by SINAN at http://tabnet.datasus.gov.br/cgi/tabcgi.exe?sinannet/animaisp/bases/ animalsbrnet.def: Region (North); Federation Unit (Acre; Amapá; Amazonas; Pará; Rondônia; Roraima and Tocantins), year and month of the accident; time elapsed between the accident and medical assistance and; the type of snake involved. The correlation being carried out between the year in which the accidents occurred and the other factors of interest in relation to these. In addition, throughout the research, “Snake” was selected in the topic, “Type of accident”.
RESULTS
In the period between January 2009 and December 2019, 313,139 cases of snakebites were recorded in Brazil, 101,565 of which occurred in the North Region. The distribution of reported cases per year in that region is shown in Figure 1.
Figure 1. Shows the number of cases of snakebites in the North of Brazil between 2009 and 2019.
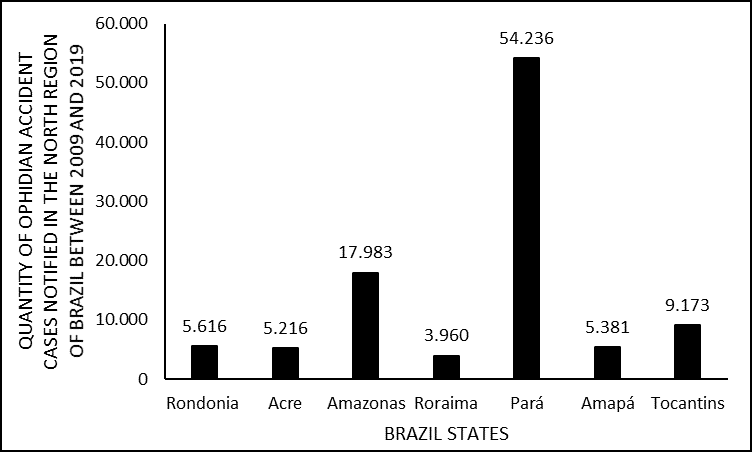
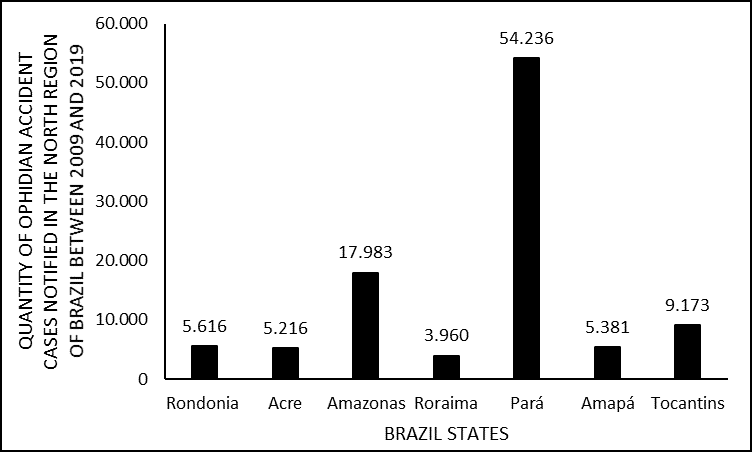
In the decade studied, it is still possible to infer the distribution of cases by Federative Unit, showing that despite the accidents occurring in the same Region, there is a considerable disparity in the number of notifications. Evidenced, for example, by the fact that Roraima registered 3,960 cases (3.90 %%); while Pará obtained 54,236 (53.40%), in the same period. Data were also obtained from other states in the North Region in the same decade, namely: Rondônia with 5,616 (5.53%); Acre with 5,216 (5.14%); Amapá with 5,381 (5.30%; Tocantins with 9,173 (9.03%) and; Amazonas with 17,983 (17.71%) reported cases (figure 2).
Figure 2. Shows the number of cases of snakebites in the North of Brazil between 2009 and 2019, by states in Brazil.
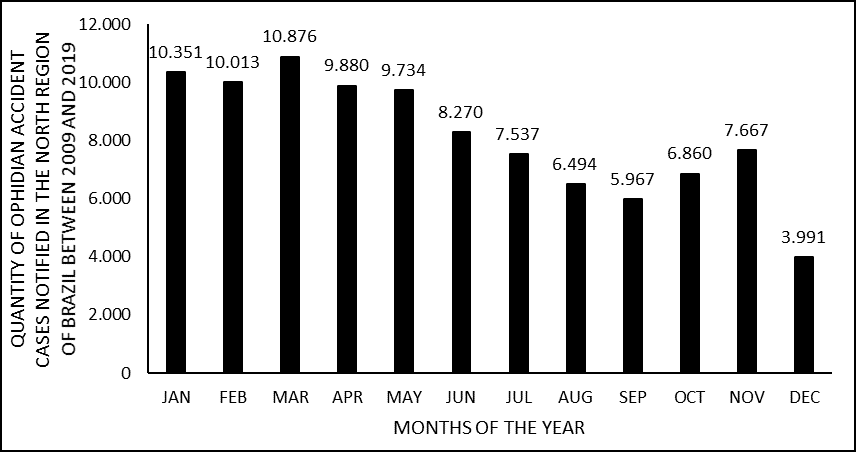
Regarding the characterization of accidents in relation to the environment, the distribution of accidents was verified according to the months of the year. In January there were 10,351 cases; February was 10,013; March 10,876; April 9,880; May 9,734, with significant decreases as of June, which presented 8,270 cases; in July there were 7,537 and; followed by August with 6,494. Reaching the lowest number of cases in September with 5,967, however with the progressive increase in cases from October with 6,860; November 7,667 and December with 7,916, as shown in percentage in figure 3.
Figure 3. Shows the number of cases of snakebites in the North of Brazil between 2009 and 2019, by months of the year.
From these reported cases, some other data of fundamental importance for the epidemiological characterization of the profile of people who suffered snakebites during that period were also checked. Such as the sex and age of the victims.
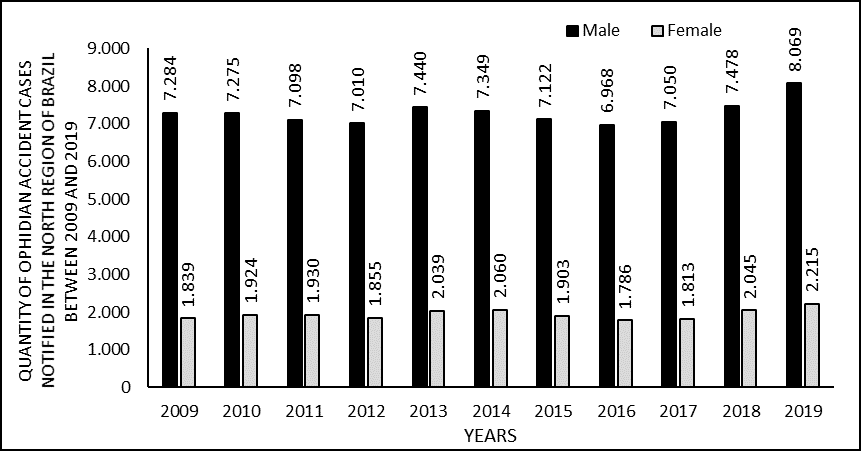
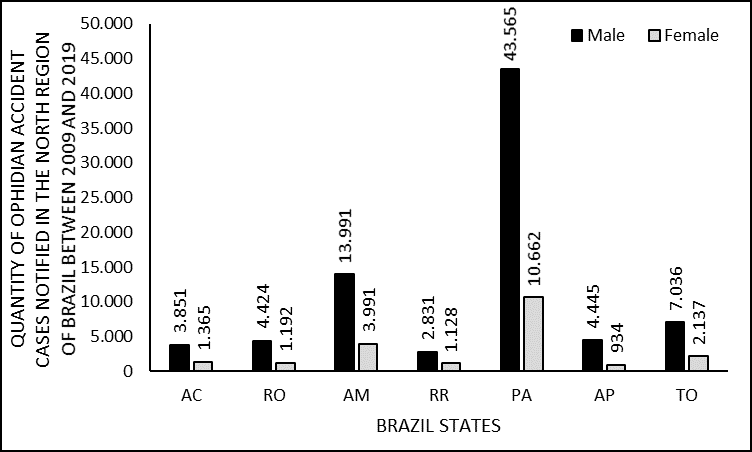
Regarding the distribution between the victims’ genders, it can be seen that of the 101,565 cases, 21,409 (21.1%) occurred with women, while 80,143 (78.9%) with men. Figure 4 shows the distribution of cases by gender, by year (2009 to 2019) in the North. Figure 5 shows the percentage distribution of accidents in relation to the victim’s gender, organized according to the notification UF, covering the entire period from 2009 to 2019.
Figure 4. Shows the number of cases of snakebites in the North of Brazil between 2009 and 2019, by gender.
Figura 5. Mostra a quantidade de casos de acidentes ofídicos na região Norte do Brasil entre os anos de 2009 e 2019, por gênero, por estados do Brasil.
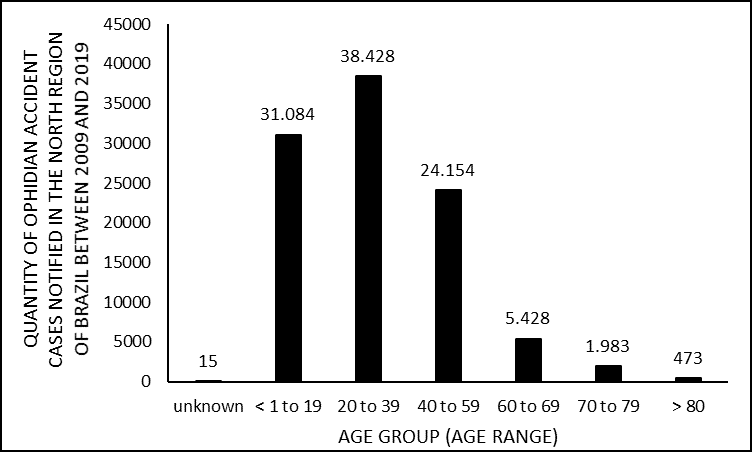
As for the percentage distribution of cases in relation to the affected age group, there were 15 cases without proper identification (ignored); 1200 cases with children under 1 year; 1,881 cases with patients between 1 and 4 years; 5,832 cases between 5 and 9 years; 10,299 with children aged 10 to 14 years, with the increasing number of cases to 11,872 in individuals aged 15 to 19 years. Reaching the peak of 38,428 cases in the 20 to 39 age group; presenting 24,154 cases in the range of 40 to 59 years, with a significant drop to 3,275 cases from 60 to 64 years; followed by 2,153 cases between 65 and 69 years old; 1,983 accidents among people aged 70 to 79 and; 473 cases in those over 80 years of age (figure 6).
Figure 6. Shows the number of cases of snakebites in the North of Brazil between 2009 and 2019, by age group.
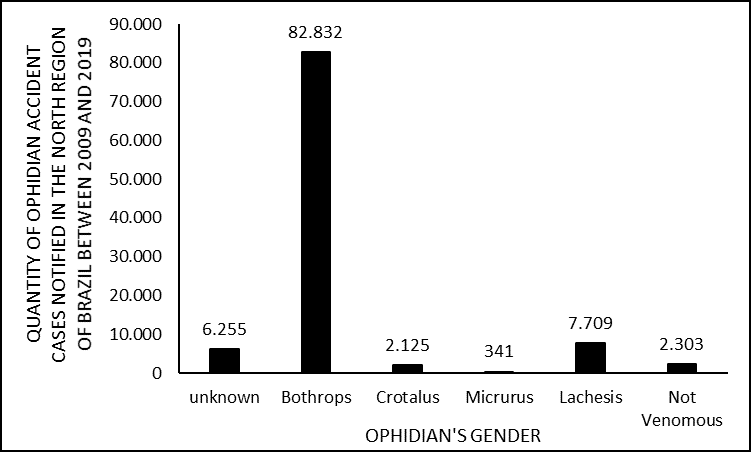
Regarding the types of snake involved, it was found that 6,255 did not have the identified type (ignored), while 82,832 were attributed to the Bothrops genus, 2,125 to the Crotalus genus, 341 to the Micrurus genus, 7,709 to the Lachesis genus, and 2,303 were identified. as accidents with non-venomous snakes; as shown in figure 7.
Figure 7. Shows the number of cases of snakebite accidents in the North of Brazil between 2009 and 2019, by type of snakebite.
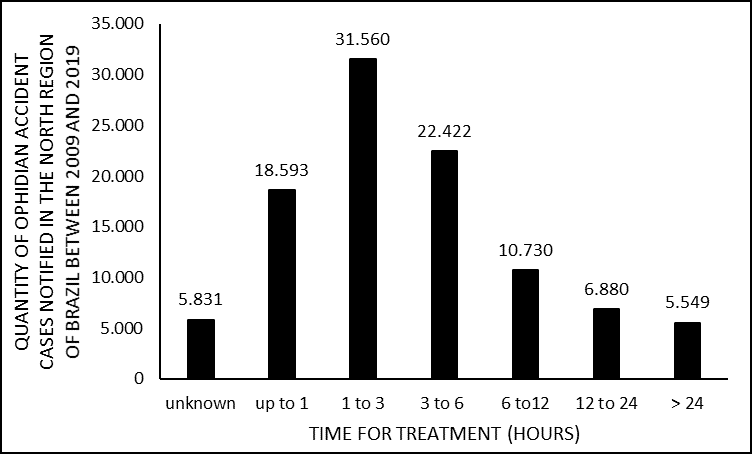
In 5,831 notification forms, the time to attendance was not filled (ignored); in 18,593 it was up to 1 hour; 31,560 people took between 1 and 3 hours; in 22,422 it was 3 to 6 hours; in 10,730 it was 6 to 12 hours; in 6,880 it was 12 to 24 hours and; 5,549 people took 24 hours or more to get care (figure 8).
Figure 8. Shows the number of cases of snakebites in the Northern region of Brazil between the years 2009 and 2019, according to the time for treatment, in hours.
DISCUSSION
According to the Epidemiological Bulletin of the Ministry of Health (BRASIL, 2019), accidents involving venomous animals in Brazil constitute the second largest cause of human poisoning, the first being represented by intoxication due to the use of medicines. The magnitude of this problem is shown in Graph 1, which shows the annual distribution of 101,565 cases recorded in the North Region during the decade from 2009 to 2019, of which 465 patients died, thus representing a lethality of 0.45%.
It is possible to notice that, even with this high number of cases and the clear relevance of the disease, the data is, in large part, incomplete, due to the failure to identify the snake that caused the accident and / or in the care of patients due to lack or low quality of notifications, which, although mandatory in the country, do not reflect the existing reality, which makes the real dimension of this problem difficult (MACHADO, 2018).
This fact is shown in Graph 2, in which it is possible to verify that the State of Amazonas, with greater extension and with a large area of preserved forest, represents only 17.7% of the notified cases. Like BORGES et al. (1999) also found, stating that this underreporting may be the result, among other factors, of difficulties in accessing health services in that region.
Another possible obstacle, noted by Machado and Bochner (2012) is the low importance given by health professionals to notifications of diseases that, despite being mandatory and fundamental to public health, affecting even the distribution of serum and the better use of public resources , are still seen as a mere bureaucratic activity, sometimes being relegated to the background, and / or carried out by an administrative employee, with the simple purpose of meeting the requirement to submit a notification to the system.
Accidents were more frequent between the months of January to May (graph 3), coinciding with periods of higher rainfall and temperature, as well as the increase in agricultural activity in the North Region. Studies indicate that there is a direct relationship between the increase in snakebite accidents and the season for agricultural activity (PINHO et al., 2004; NASCIMENTO, 2000).
This hypothesis has also been supported by the fact that rainfall would raise water levels in rivers, causing the snakes that inhabit the regions close to these margins to migrate in search of solid land, therefore, with the decrease of this territorial space, it increases if contact with human populations, which would facilitate the occurrence of accidents (MORENO et al., 2005; PARDAL et al., 1995).
4 and 5) and the distribution by age group (graph 6) characterize the profile of those affected by these disorders. In the present study, there was a higher frequency between 20 to 39 and 40 to 59, affecting, therefore, most men, of working age.
Moreno et al. (2005) found that the majority of accidents involve male people, rural workers, from 10 to 29 years old, probably due to the greater frequency with which this group develops activities, mainly in agriculture and extraction. Soon, this occupational segment would be more exposed to snakes and, consequently, to accidents. Machado and Bochner (2012) corroborate these findings that found that patients of rural origin, or who reported agricultural activity, have an increased risk of snakebite accidents, therefore, identified as a high risk group. Among the main factors that define these accidents, we can highlight the link with economic activities related to the countryside, forest and water, thus being able to be classified mostly as a work accident (BRASIL, 2014).
The distribution of accidents by gender of snakes is important because it helps in the more precise indication of the antivenom to be administered and the conduct to be taken. In addition to enabling the recognition of species of medical relevance at the regional level (BRASIL, 2001).
In this study, Bothrops snakes (82%) have the highest number of accidents (82%) followed by Lachesis snakes (7%) (graph 7). As noted by Borges et al. (1999), the results obtained do not differ from those observed by other authors with regard to the genus of the snake Bothrops responsible for the largest number of snakebite accidents with poisoning.
Ophidian accidents are classified according to the genus of the snake, being named Bothrops, Crotalus, Lachesis and Micrurus. This division has essential clinical value, since the poisons found in these four groups of snakes have different behaviors in the patient, their identification being, therefore, determinant in the conduct and follow-up of the case (BARRAVIERA, 1992).
These genera are related, respectively, among others, to the species popularly known as: jararacas, jararacussu; rattlesnakes; surucucus; and true corals (MELGAREJO, 2003). Each genus presents a clinical picture after the accident, depending on the amount of poison inoculated. Botropic and laquetic accidents generally present pain, edema, ecchymosis and erythema, as well as local complications, such as: cellulite, abscesses, compartment syndrome and, if left untreated, can progress to limb amputation (OTERO PATIÑO, 2009).
In crotalic accidents, edema and paresthesia can be found, although they do not usually present significant local changes (AMARAL, 2001). Systemic manifestations are found, such as renal and neurological alterations, such as paresthesia, or even paralysis with craniocaudal progression, starting with ophthalmoplegia and palpebral ptosis, which can cause acute respiratory failure, through respiratory muscle paralysis (AMARAL, 2001; BRASIL, 2001).
Accidents with species of the genus Micrurus may present with mild local manifestations such as paresthesia and pain of varying intensity with or without irradiation, which may even be absent. In a systemic character, acute myasthenia may occur with eyelid ptosis and objective decrease in muscle strength, with no signs of paralysis in moderate cases. In severe cases, the patient may show signs of severe muscle weakness and muscle paralysis that can progress to acute respiratory paralysis (BRASIL, 2014).
The time to attend to snakebite accidents (graph 8), which in the period under analysis was mostly up to 3 hours after the bite, followed by 6 to 12 hours after the bite. It is also observed that patients who are victims of bites in the limbs, who use tourniquets, who were seen more than six hours after the accident, or who received incorrect administration of antiophidic serum, had a worse prognosis (JORGE, RIBEIRO, 1990).
An important guideline is to seek medical attention, which should be as soon as possible. Regarding the care of victims, the prognosis is generally good in accidents classified as mild and moderate and in patients seen in the first six hours after the bite (BRASIL, 2001).
CONCLUSION
The relevance of snakebite accidents was found, mainly in the North Region of the country, and in the registered cases the relationship between snakebite and the rainy season was clear, noting that in the months from January to May there is a significant increase in the number of cases, corresponding precisely to the periods in which rainfall is increased, whether due to the displacement of snakes in search of shelter or because it coincides with periods of important agricultural activity.
This relationship between snake accidents and agrarian activity is so relevant that this condition could be classified as an occupational disease. In the present study, this association is clear when one realizes that the majority of accidents occurred with male patients (78.9%), and in working age (50%) between 20 and 59 years old.
The main genus of snake related to accidents in the present study is Bothrops, representing 81.56% of the cases. Another factor observed is that 49.38% of the patients were seen up to 3 hours after the accident, which is important for a good prognosis, however, 22.79% still took more than 6 hours to be seen, which reduces the chances of a favorable outcome.
It should also be noted that despite the significant number of reported cases, this condition is not always registered, due to this underreporting, access to reliable data is compromised. In addition, the lack of demand for specialized care potentially leads to a worse prognosis of the condition, often resulting from misconduct such as the use of tourniquets, teas and mistaken home measures. Thus reaffirming the need for medical care and adequate notification.
REFERENCES
AMARAL, C.F.S. et al. Manual de de diagnóstico e tratamento de acidentes por animais peçonhentos. 2 ed. Brasília. Ministério da Saúde, Fundação Nacional de Saúde, 2001.
BARRAVIERA, B. O ensino dos acidentes por animais peçonhentos nas escolas médicas brasileiras. Revista da Sociedade Brasileira de Medicina Tropical 25(3): 203-204, jul-set, 1992.
BORGES, C. C.; SADAHIRO, M.; SANTOS, M. C. Aspectos epidemiológicos e clínicos dos acidentes ofídicos ocorridos nos municípios do Estado do Amazonas. Rev. Soc. Bras. Med. Trop., Uberaba , v. 32, n. 6, p. 637-646, Dec. 1999. Disponível em:<http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0037-86821999000600005&lng=en&nrm=iso>. Acesso em 18 jan 2020.
BRASIL. Ministério da Saúde. Manual de diagnóstico e tratamento de acidentes por animais peçonhentos. Brasília: Fundação Nacional de Saúde; 2001.
BRASIL. Ministério da Saúde. PROTOCOLO CLÍNICO. Acidente por serpente da família Elapidae, gêneros Micrurus e Leptomicrurus “Coral verdadeira”. 2014. Disponível em: http://www.saude.gov.br/images/pdf/2014/marco/13/Protocolo-clinico-Acidente-por-serpente-da-familia-Elapidae.pdf. Acesso em 11 jun 2020.
BRASIL. Ministério da Saúde. Boletim Epidemiológico: Acidentes de trabalho por animais peçonhentos entre trabalhadores do campo, floresta e águas, Brasil 2007 a 2017. Secretaria de Vigilância em Saúde; 2019.
GUTIÉRREZ, J.M.; CALVETE, J.J.; HABIB, A. G.; HARRISON, R.A.; WILLIAMS, D. J.; WARREL, D. A. Snakebite envenoming. Nature Rewies: Disease Primers, San Jose, Costa Rica, v. 3, n. 17063, 14 set 2017. DOI https://doi.org/10.1038/nrdp.2017.63. Disponível em: https:www.nature.com/articles/nrdp201763. Acesso em 02 de fev 2020
JORGE, M.T.; RIBEIRO, L.A. Acidentes por serpentes peçonhentas do Brasil. Rev Assoc Med Bras.; 36(2):66–77; 1990.
MACHADO C.; BOCHNER, R. A informação dos acidentes crotálicos no Estado do Rio de Janeiro, 2001 a 2010. Gaz Med Bahia ;82(1):78–84; 2012.
MACHADO, C. Acidentes ofídicos no Brasil: da assistência no município do Rio de Janeiro ao controle da Saúde Animal Instituto produtor de soro antiofídico; Rio de Janeiro; 2018.
MELGAREJO. A. R. 2003. Serpentes peçonhentas do Brasil. Pp. 33-61 In: Animais peçonhentos no Brasil: biologia, clínica e terapêutica dos acidentes. Cardoso et al. (Orgs.). Sarvier, São Paulo – SP.
MORENO, E.; ANDRADE, M. Q.; SILVA, R. M. L da; NETO, J. T. Características clínicoepidemiológicas dos acidentes ofídicos em Rio Branco, Acre. Rev. Soc. Bras. Med. Trop., Uberaba , v. 38, n. 1, p. 15-21, Feb. 2005 . Disponível em: <http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0037-86822005000100004&lng=en&nrm=iso>. Acesso em 18 jun 2020.
NASCIMENTO, S. P. Aspectos epidemiológicos dos acidentes ofídicos ocorridos no Estado de Roraima, Brasil, entre 1992 e 1998. Cad. Saúde Pública, Rio de Janeiro , v. 16, n. 1, p. 271-276, Jan. 2000 . Disponível em: <http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102-311X2000000100031&lng=en&nrm=iso>. Acesso em 18 jun 2020.
OTERO-PATIÑO, R. Epidemological, clinical and therapeutic aspects of Bothrops asper bites. Toxicon, v.54, p 998-1101, 2009.
PARDAL, P. P. O. Aspectos epidemiológicos de 465 acidentes atendidos no HUJBB-Belém, Pará, no período de 1993-1994. In: Congresso da Sociedade Brasileira de Medicina Tropical, 31, São Paulo, 1995. livro de Resumos, resumo 340, 1995, p. 170.
PINHO, F..M.O.; WHO, P.I.D. Ofidismo. Rev. Assoc. Med. Bras. 2001; 47(1):24-9.
PINHO, F.M.O; OLIVEIRA, E.S.; FALEIROS, F. Acidente ofídico no estado de Goiás. Rev. Assoc. Med. Bras., São Paulo , v. 50, n. 1, p. 93-96, 2004 . Disponível em:<http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-42302004000100043&lng=en&nrm=iso>. Acesso em 16 jun 2020.
WEISS, M.B.; PAIVA, J.W.S. Acidentes com animais peçonhentos.1 Ed. Rio de Janeiro- RJ: Thieme Revinter Publicações Ltda, 2017. p. 36-37.
WHO. WORLD HEALTH ORGANIZATION (Geneva, Switzerland). Snakebite envenoming: A strategy for prevention and control. Geneva: [s. n.], 2019. 55 p. E-book.
[1] Student of the Medical Course at the Federal University of Amapá (UNIFAP).
[2] Student of the Medical Course at the Federal University of Amapá (UNIFAP).
[3] Student of the Medical Course at the Federal University of Amapá (UNIFAP).
[4] Biologist, PhD in Theory and Research of Behavior, Professor and researcher of the Graduate Program in Professional and Technological Education (PROFEPT), Federal Institute of Amapá (IFAP).
[5] Biologist, Doctor in Topical Diseases, Professor and researcher of the Physical Education Course at the Federal University of Pará (UFPA).
[6] Theologian, PhD in Psychoanalysis, researcher at the Research and Studies Center Advanced – CEPA.
[7] Biomedical, PhD in Tropical Diseases, Professor and researcher of the Course of Medicine at the Federal University of Amapá (UNIFAP).
Submitted: September, 2020.
Approved: September, 2020.